Patients miss out on 1.8million days of care - as nurses battle with unsuitable products


New insight indicates the average patient in a hospital or care home setting with the inability to self-manage their condition, will demand 75 minutes of a carer’s time every day, covering up to five changes.
But those caring for these patients warn this is 78 per cent – or 42 minutes – longer than would be necessary, if better fitting products were procured.
Advertisement
Hide AdAdvertisement
Hide AdOf the 500 nurses and carers polled, 49 per cent admit they are not fulfilling the needs of their patients because too long is spent trying to work with improper materials.
And others said their duties are hampered by patients who have not benefited from a personal assessment, which is often replaced with a ‘one size fits all’ approach (53 per cent).
With an improved approach to continence services, procurement practices, and better patient services, nurses and carers predict they could carry out two fewer changes a day, reducing each change by four minutes.
Richard Maddison, spokesman for hygiene and health company Essity, which has carried out multiple studies – including an NHS driven pilot– into incontinence care and provision of products, said: “This is another example of the false economy procurement process within the NHS driven by a government that is failing to look at the bigger picture.
Advertisement
Hide Ad“Healthcare professionals are crying out for products that are fit for purpose, that enable them to do their jobs more efficiently, and that would actually save the NHS time and money as a result.
Advertisement
Hide Ad“The irony is that by focusing on value rather than cost during the procurement process, the government could improve patient outcomes, free up nurses so that they can provide better care to more patients and save millions of pounds that are being squandered on lower quality products. It’s a win-win situation.”
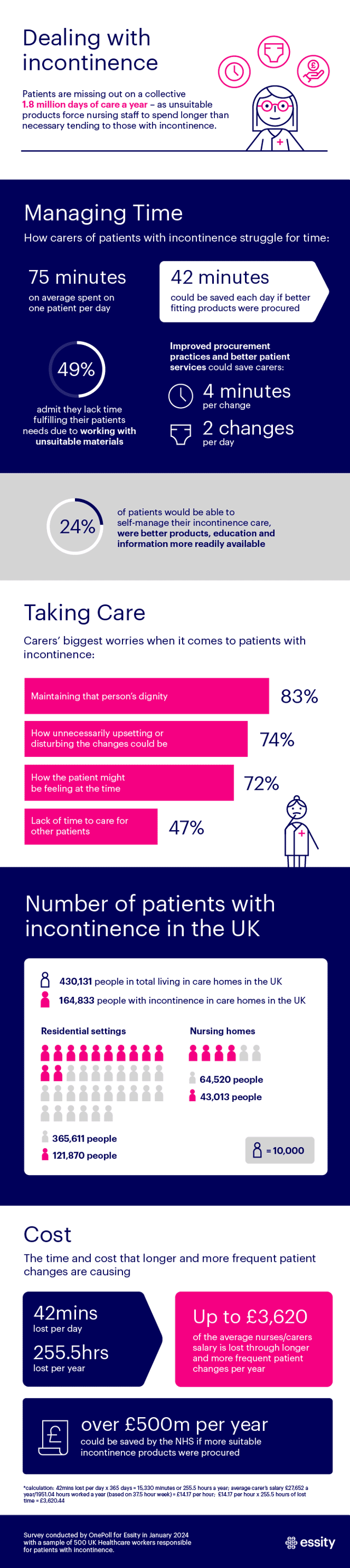

The study revealed the average incontinence carer polled brings home an average annual salary of £27,652.
Which means longer and more frequent patient changes are effectively costing up to £3,620.44 per carer, per year.
Advertisement
Hide AdAnd this leads to 47 per cent worrying about other patients who might not end up receiving the broader care they need, because they are spending too much time providing wrap around care to patients with incontinence.
Those questioned via OnePoll believe 24 per cent of patients would be able to self-manage their incontinence care, were better products, education and information more readily available.
Advertisement
Hide AdAnd for those directly responsible for patient changes, 83 per cent admitted their biggest concern was maintaining the dignity of that person.
While 74 per cent worry how unnecessarily upsetting or disturbing the changes could be, or how the patient might be feeling at the time (72 per cent).
Advertisement
Hide AdMore than one in 10 (12 per cent) have real concerns about bed blocking – again, something they feel could be avoided and which circles back to the inability to provide care to a wider patient network.
Tracy Evans, an NHS continence clinical nurse specialist, who participated in one of Essity's studies added: “Patient dignity is of the utmost importance, but this becomes more difficult to manage with frequent changes.
“There are two things which could ultimately lead to shorter, more manageable incontinence changes – an individualised holistic assessment leading to a personal plan for every patient, and a more sophisticated procurement programme liked to evidence based holistic care.
“Both of these would immediately benefit those trying to manage their incontinence, and in turn, free up our nurses to provide care for others who desperately need their time.”