High Peak health campaigner asks women to share their stories to help improve gynaecology care
This article contains affiliate links. We may earn a small commission on items purchased through this article, but that does not affect our editorial judgement.
and live on Freeview channel 276
Birch Vale resident Maddy Howarth, 26, launched the online initiative ‘Let's Change It. Period.’ last year to push for changes in patient care, saying the current system leaves women facing years of agony and uncertainty.
It is a struggle she knows all too well. From the age of 13, she lived with crippling pain which by early adulthood forced her to give up her job and home. After an eventual diagnosis of endometriosis and adenomyosis, and a decade of failed remedies, Maddy opted to have a hysterectomy.
Advertisement
Hide AdAdvertisement
Hide AdShe said: “There’s an issue with the entire system around women’s health in the NHS. If it’s to do with periods or the womb we are treated for fertility, not pain.


“It’s not seen as the best outcome to get a patient fit and healthy. The priority is fertility and that comes at cost to quality of life, careers and mental health. It’s horrendous that this is still the case in 2022.”
She added: “If I can can collect other women’s stories and show there is a pattern they will have to listen and do something.”
With support from High Peak MP Robert Largan, Maddy submitted a detailed account of the treatment she received and recommendations to NHS Derby and Derbyshire Clinical Commissioning Group (CCG) – but the response has brought more frustration.
Advertisement
Hide AdFirst Mr Largan received a letter, in which executive medical director Dr Steven Lloyd wrote: “Unfortunately, given the current extreme pressures on the NHS, the current pathway for endometriosis services is not currently a transformation priority for the NHS in Derbyshire.”


Advertisement
Hide AdAfter the Advertiser began asking questions Maddy also eventually received a response, just as discouraging.
She said: “It felt like we were being fobbed off. I was asked to send my personal story to the patient feedback service, and it was just ignored.
“I know the NHS is under pressure, but Covid didn’t exist five years ago and the narrative was no different. Women’s health is never deemed a priority, that’s why it’s in a dire state.”
Advertisement
Hide AdDespite the framing of “transformational priorities”, Maddy’s top recommendation appears relatively straightforward.


She said: “What I’m suggesting isn’t about restructuring at all. It’s a simple change to the way GPs refer women to gynaecologists. If I had a heart problem I wouldn’t be sent to a breathing specialist but that’s essentially what’s happening.
Advertisement
Hide Ad“GPs have a list ordered by location, so the patient could be referred to someone who is not a specialist in their condition. Another girl told me how she had been referred to a gynaecologist who had never treated anyone with endometriosis, even though the same hospital had a specialist centre for the condition.”
She added: “When a woman has stage four endometriosis, they really need a specialist but they may be referred to someone who can’t help. The patient thinks they are in the best hands, but they are just being put through multiple investigative surgeries and different medications at a young age.
Advertisement
Hide Ad“By adding information about specialisms to GPs’ referral lists you could ensure women are being seen by the correct people.”
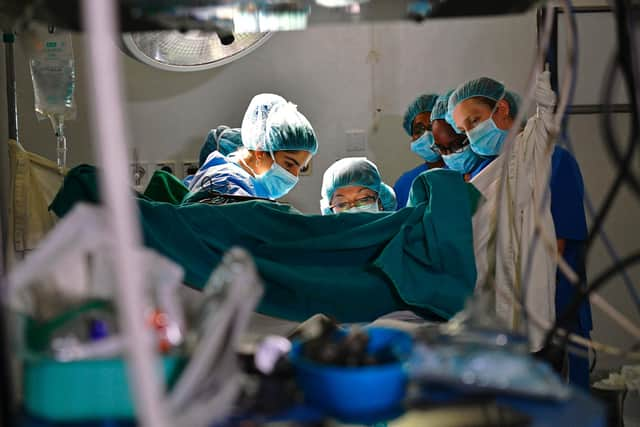

The CCG has said it is for hospital departments to allocate patients to the most appropriate specialist, but its response to Maddy’s recommendations also highlights other significant issues for High Peak patients.
While all her primary care was delivered in Derbyshire, the CCG’s contracting arrangements meant surgical procedures were delivered by a specialist at the private Spire Regency Hospital in Macclesfield.
Advertisement
Hide AdIn response to Maddy’s feedback, Dr Lloyd wrote: “[Your patient story] highlighted that the inpatient care, investigations and treatment, including hysterectomy, were likely performed outside of Derbyshire. This unfortunately precludes the Derbyshire consultant teams from commenting specifically on your experience.”
Advertisement
Hide AdThe organisation has yet to explain why it cannot comment on services it was responsible for commissioning, or how other patients can have confidence in treatment under similar circumstances, but Maddy is now pursuing a formal complaint.
She said: “About 20 per cent of my treatment was delivered in Cheshire, but they’ve focused on that as a way to dismiss the rest of my story and not investigate it.
“The CCG has a responsibility if they are referring patients on. I’m offering feedback which should be useful for them to learn and improve, but they are just completely ignoring it.”
A spokesperson for NHS Derby and Derbyshire said: “The CCG has received a formal complaint, this is being investigated in line with our procedures and we will provide a response in due course.
Advertisement
Hide AdAdvertisement
Hide Ad“It would be inappropriate to discuss further details of this communication with anyone other than Madeleine, as it relates to her care and the investigation is still underway.”
They added: “We recognise that women with endometriosis face many challenges in the management and treatment of their condition, and we understand the severe impact it can have on their lives.
“We welcome feedback on ways services can be improved, and encourage women to see their GP if they have symptoms of endometriosis. However, some practices are providing only urgent appointments at present due to staff shortages.”
While Maddy’s struggle for change continues, there is some hope on the horizon in the shape of a new Government strategy for improving women’s healthcare, which acknowledges a lot of the issues she has experienced and makes the case for systemic changes.
Advertisement
Hide AdMaddy said: “This will go down as the generation who had the science to improve women's health, but chose not to. The Women's Health Strategy is the first step to changing this narrative, however we are leaps away from closing the gender health gap on women's health beyond fertility.”
Advertisement
Hide AdIf you have a story to share with Maddy as part of her campaign, contact her via facebook.com/letschangeitperiod or instagram.com/letschangeitperiod.